Inventing soft things to solve hard problems
Xuanhe Zhao first displayed an interest in science when he accompanied his father, a truck driver in Liaoning province, on trips to farms in northern China. He was five years old.
“My father used to transport produce from rural farms to cities with a truck and took me along for the ride,” says Zhao, now an MIT professor of mechanical engineering. “I got close contact with many farm animals and asked lots of questions: ‘Why do chickens give us eggs, but cows give us milk?’ My father would answer these questions during the trips and let me read scientific books later.”
It was the start of a journey that has led him to become one of the most prolific engineering researchers at MIT.
When people ask him what his lab does, Zhao says, “We invent soft things to solve hard problems.”
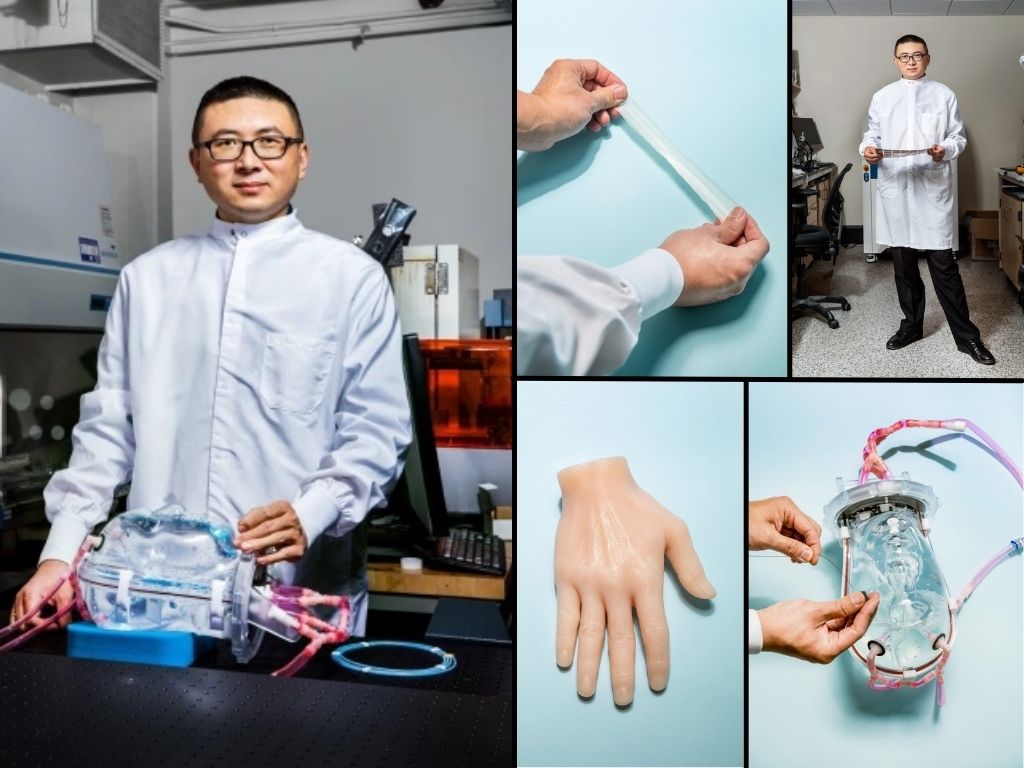
Zhao works with hydrogels, which are polymers that can absorb a large volume of water while still retaining their shape. In effect, his lab is producing synthetic versions of the materials that constitute most of our body. “Except for nails, teeth, and bones,” he says, “all other components of the body are hydrogels.” They make up our muscles, tendons, ligaments, cartilage, and brain.
Among other things, his lab has invented a tough yet stretchy hydrogel modeled on a lobster’s underbelly; 3D-printed structures made of magnetically infused ink that can roll, crawl, twist, jump, and grab; and nearly invisible hydrogel robots that can move around underwater, and even catch and release live fish.
But it’s the ongoing initiatives that show the true ambitions of his lab.
Preventing stroke damage
In the United States, nearly 800,000 people a year experience strokes, which cause a loss of blood to the brain through bleeding or clots. They are a leading cause of disability and the fifth leading cause of death.
Currently, physicians treating someone with a blood clot in the brain insert a catheter into an artery, guide it to the affected area, and remove the clot with suction or a stent. An interventional radiologist uses x-ray fluoroscopy to guide the catheter to the right spot, manually negotiating the twists and turns in the labyrinthine network of the brain’s circulatory system.
“Except for nails, teeth, and bones, all other components of the body are hydrogels.”
The skill required to swiftly insert a catheter and remove a clot takes years of experience. But highly experienced physicians are clustered at the most advanced hospitals; they’re often unavailable at smaller hospitals or in rural areas. What’s more, working with x-rays is dangerous for doctors. Radiologists wear lead vests and other protective clothing, but they still have a higher risk than other physicians of developing cancer and cataracts from the repeated exposure to radiation.
Zhao’s invention is designed to address both of these concerns.
His device uses a surgical robot to guide the catheter through the body. The catheter is made of an elastomer (a stretchy polymer) that is magnetically sensitive, so that magnets placed near the patient’s body can control its movement into and through the brain. The doctor can use a joystick and watch the catheter’s progress with x-ray imaging but doesn’t have to be in the same room as the patient, reducing the radiation exposure.
“Because it is an autonomous system, the doctor conceivably could even be in another city,” Zhao says.
Aman Patel, a Massachusetts General Hospital neurosurgeon who works with Zhao, says the system has performed well in early tests on a synthetic model of the brain, although for him it wasn’t as quick as using a manually guided wire. But interestingly, surgical fellows using the MIT device were almost able to equal his time—because with its help, they didn’t need his thousands of hours of surgical expertise to approach his level of skill.
Patel estimates that human clinical trials of Zhao’s device are at least a couple of years away.
Replacing sutures
Another of Zhao’s innovations is a quick-sealing tape that can replace surgical sutures and staples, in conjunction with a gel that can instantly stop severe bleeding.
Ever since surgery became a mainstay of modern medicine, stitches and, more recently, staples have been the two techniques doctors have used to close incisions. Most of the time, these work fine, says Christoph Nabzdyk, an anesthesia and critical care specialist at the Mayo Clinic in Rochester, Minnesota. But as America’s population ages, more and more older patients are undergoing surgery, and in general, their skin and other tissues don’t heal as fast as those of younger patients.
Elderly patients aren’t the only ones at risk from incisions that heal slowly or even reopen. People who have received chemotherapy and radiation, or those with autoimmune diseases, also heal more slowly. It’s such a problem, Nabzdyk says, that some surgeons won’t do certain high-risk operations on these patients “because they’re too nervous about leakage, since it can be a death sentence.”
One potential solution is some sort of surgical patch, which is what Zhao’s lab has been working on with Nabzdyk as a clinical collaborator.
The key hurdle is that blood, water, or other moisture at the site of an incision makes it difficult, if not impossible, for most surgical adhesives to form a bond. Zhao’s solution? A tape made of hydrogels that suck up the moisture before the adhesive bonds. The biocompatible tape can stay in place indefinitely and is eventually absorbed by the body’s tissues.
Nabzdyk’s lab performed experiments on pigs by poking two holes in their colons, which are particularly prone to infection, and then using the surgical tape to seal the wounds. He says all five pigs that underwent the procedure grew, ate normally, and thrived.
To make the surgical tape even more useful, Zhao’s lab also ensured that it would be easy to remove.
They accomplished that by introducing disulfide linker molecules to the tape material. Then, to break the adhesive bonds, they spray on a mixture that includes sodium bicarbonate (baking soda). After about five minutes, the tape comes right off, without tearing any of the tissue underneath.
“This is like a painless Band-Aid for internal organs,” says Zhao. “You put the adhesive on, and if for any reason you want to take it off, you can do so on demand, without pain.”
Even more promising for applications in the near future is a version of the hydrogel that can be squeezed into cuts and gashes as a wound-sealing glue.
To develop the glue, Zhao’s lab took its inspiration from barnacles, creatures that can attach to ships’ hulls and even the sides of whales underwater without losing their grip. The research showed that the sticky substances in barnacles are bathed in an oily substance that repels water and contaminants, allowing a tight bond in their wet environment.
“He has such a wide bandwidth to address so many challenges, from medicine to engineering.”
Zhao and his group started with the same compounds that they use to create the surgical tape, but they added chitosan, a sugar derived from shellfish skeletons. The researchers froze the mixture into sheets and then ground them into tiny particles that they mixed with silicone oil.
When they applied the resulting paste to bleeding tissues, the oil repelled the water and blood. Within 15 to 30 seconds, the gel had formed a tight bond with the underlying tissue, stopping further bleeding.
In a paper published in Nature Biomedical Engineering, Nabzdyk, Zhao, and their team said the gel had worked successfully in pigs that had been injected with the blood thinner heparin and then given liver injuries. Existing surgical glues did not work in these animals because those glues rely on forming clots, and the heparin prevented that. The Zhao lab’s paste sealed the wounds within seconds.
“We found you can have brisk arterial bleeding and it will still seal; it will form this sort of cap,” says Nabzdyk. “The oil in the paste just pushes the liquid away.”
Nabzdyk and Zhao have formed a company called SanaHeal to promote the new surgical glue. Nabzdyk thinks it could have uses ranging from closing surgical incisions to treating battlefield wounds or gunshot and other traumatic injuries.
“One of the nice things about it is that the chemicals we use are individually already FDA-approved and are very cheap,” Nabzdyk says.
Inflatable hand
For the more than 5 million upper-limb amputees around the globe, scientists have developed increasingly advanced prosthetic limbs. Modern prosthetics have sensors that pick up signals from residual muscles and translate them into movements controlled by motors.
But these plastic and metal marvels, which can cost more than $10,000, are out of reach for many who need them. The World Health Organization estimated in 2017 that there were 30 million amputees worldwide, and 75% of those living in developing countries don’t have access to prosthetics at all.
Those disparities inspired Zhao’s lab to work with Shanghai Jiao Tong University to develop a cheap, inflatable prosthetic hand. The result costs about $500 and weighs about half a pound—half the weight of some advanced prosthetic hands. It is operated pneumatically with air pumped into the fingers.
By attaching sensors that detect nerve signals in the residual limb and asking the wearers to imagine different hand positions, the researchers can train a prototype of the inflatable hand to achieve five different positions—including pinching motions, a balled fist, and an upraised palm. A video with one skilled tester showed him drinking a glass of wine, petting a cat, eating potato chips, and unzipping a satchel.
Zhao says the inflatable hand should ultimately be able to achieve 10 different positions. Each of the inflatable fingers has a sensor that can be attached to different parts of a person’s arm. The prosthetic doesn’t duplicate the sensation in the original hand, but it gives users a set of signals that allow them to know what the device is doing and “feel” its position without looking at whatever it is touching.
Building his skills
Zhao got his electrical engineering degree in 2003 from Tianjin University in China, where he learned the basics of circuit design. Three years later, he got his master’s in material engineering at the University of British Columbia, where he learned the basics of materials design. After earning his PhD in mechanical engineering at Harvard University, he did a postdoc in biomedical engineering, “and so I closed the loop on many different disciplines,” he says.
Both Patel and Nabzdyk say a prominent feature of Zhao’s lab is how much freedom and responsibility he gives to his doctoral and postdoctoral students. “He’s been an easygoing guy to work with,” Patel says.
“He has such a wide bandwidth to address so many challenges, from medicine to engineering,” adds Nabzdyk. “He is still very young and yet has had a meteoric rise thanks to his unbelievable dedication. He also has the ability to recruit some of the most brilliant postgrads I’ve seen, so it’s really fascinating to see how he is able to allow trainees to have independence and yet be very goal-oriented and impactful.”
Part of that output comes from Zhao’s philosophy for running his lab.
“For my PhD students, I try to train them with broad knowledge for adhesives, actuators, and soft materials,” he says. “And then, 50% of the time we talk about what goal they want to achieve, like stroke treatment. And the other 50% of their time can be curiosity driven, so they can do random experiments that interest them.”
But Zhao, who has a three-year old and a one-year-old with his wife, a professional pianist, has never forgotten that such curiosity begins much earlier than graduate school.
“Just as when I was a boy, we are taking our daughters to farms, zoos, and nature today,” he says. “The girls ask similar questions, and I hope they too will love science and nature when they grow up.”
Rising stars of the Zhao lab
Hyunwoo Yuk, SM ’16, PhD ’21, a research scientist in Xuanhe Zhao’s lab at MIT, is one of the founders of a new company, SanaHeal, that will market a paste that can quickly stop major bleeding, as well as a surgical adhesive to replace sutures.
His research on those products was driven by a crisis in his own family. When he was getting ready to finish his undergraduate studies at the Korea Advanced Institute of Science and Technology nine years ago, his younger brother, Youngwoo, experienced a horrific fall.
Youngwoo, then 16, leaned against a rickety fence at a building in their hometown of Daegu, South Korea, and plummeted five stories. He slammed onto the surface of a garden instead of the pavement, which may have saved his life, but he broke his ankle, damaged his spine, and suffered extensive bleeding.
“Luckily, we were within a 10-minute ambulance ride to a major university hospital,” Yuk recalls, “so he survived the initial trauma. But I still remember the bleeding all over his body—it’s a scene that is hard for me to forget.”
Youngwoo was in the neurosurgery ICU for three months. He had four major surgeries to repair arterial damage, broken bones, and spinal cord damage, and then he spent another 10 months in the hospital and rehab before returning home.
“I was with him throughout the whole process along with my mother, and I got to see the marvel—and the limitations—of medical technology,” Yuk says. So it’s natural, he reflects, that he became interested in ways to stop major bleeding.
His lead role in developing a hydrogel surgical adhesive in Zhao’s lab earned Yuk the 2020 graduate award in the Collegiate Inventors Competition sponsored by the National Inventors Hall of Fame. He was also named one of Forbes magazine’s 30 under 30 in 2019.
Yuk is not the only one of Zhao’s graduate students who have won awards and national recognition.
Sarah Wu, a graduate researcher, and Jingjing Wu, a postdoctoral researcher, both in Zhao’s lab, each won a 2021 Baxter Young Investigator Award for their work on bioadhesives—Sarah for the multifunctional patch and Jingjing for the hemostatic paste.
Yoonho Kim, another Korean doctoral researcher, was the lead author in the Science Robotics paper in 2019 that outlined the magnetically guided stroke treatment wire.
The graduate students’ achievements are no surprise to Aman Patel, director of cerebrovascular and endovascular surgery at Massachusetts General Hospital, who has worked with Zhao’s team.
“What I’ve been amazed by is that he doesn’t seem to micromanage the postdocs involved in this,” Patel says. “He doesn’t feel like he needs to be involved at every step.”
Article reposted from: MIT Technology Review